Author
Dr. Nilesh Chordiya
GI & Gynaec Cancer Surgeon
MBBS, MS – General Surgery
Early Signs & Symptoms of Pancreatic Cancer: A Comprehensive Guide
Pancreatic cancer is a serious and often life-threatening disease that develops when malignant cells form in the tissues of the pancreas.
The pancreas, located deep within the abdomen behind the stomach, plays a crucial role in our body’s digestive system and hormone regulation.
It consists of two main parts: the exocrine glands, which produce enzymes that help digest food, and the endocrine glands, which release hormones such as insulin and glucagon to regulate blood sugar levels.
Several risk factors can increase an individual’s likelihood of developing pancreatic cancer, including age, family history, smoking, obesity, and chronic inflammation of the pancreas (pancreatitis).
Understanding these risk factors and being aware of the warning signs can help with early detection and improve treatment outcomes. In the following sections, we will discuss the symptoms, diagnosis, and treatment options for pancreatic cancer.
Symptoms of pancreatic cancer

- Abdominal pain: Pancreatic cancer patients often experience persistent, dull pain in the upper abdomen due to the growing tumor pressing against nerves or surrounding organs. This pain may radiate to the back and can worsen after eating or lying down.
- Jaundice: Jaundice is the yellowing of the skin and eyes caused by a buildup of bilirubin, a waste product, in the blood. In pancreatic cancer, the bile duct may be obstructed by the tumor, preventing bilirubin from being processed and eliminated. This obstruction leads to jaundice, which is often accompanied by dark urine, light-colored stools, and itching.
- Weight loss: Unintended weight loss is a common symptom of pancreatic cancer. The tumor may interfere with the pancreas’ ability to produce digestive enzymes, leading to malabsorption of nutrients and subsequent weight loss. Additionally, cancer cells use up energy reserves, further contributing to weight loss.
- Fatigue: Extreme tiredness and weakness are common among people with pancreatic cancer due to the body’s energy being diverted to fight the disease. Anemia, caused by low red blood cell counts, may also contribute to fatigue.
- Nausea and vomiting: Pancreatic cancer can disrupt normal digestion, leading to feelings of nausea and episodes of vomiting. These symptoms may be exacerbated by the tumor pressing on the stomach or blocking the flow of digested food through the intestines.
- Diarrhea or constipation: Changes in bowel habits, such as diarrhea or constipation, can occur in pancreatic cancer patients. These changes may be due to the tumor interfering with the normal function of the digestive system or as a side effect of certain treatments.
- Back pain: Similar to abdominal pain, back pain is a common symptom of pancreatic cancer. This pain can result from the tumor pressing against nerves or surrounding organs, causing discomfort in the back area.
- Blood clots: Pancreatic cancer increases the risk of blood clots forming in the veins, a condition known as deep vein thrombosis (DVT). These clots can cause swelling, pain, and warmth in the affected limb and may lead to more serious complications if they dislodge and travel to the lungs, causing a pulmonary embolism.
- Itchy skin: Itchy skin, or pruritus, is often associated with jaundice in pancreatic cancer patients. The buildup of bilirubin in the skin can cause irritation and itching, leading to discomfort and the urge to scratch.
Take action against pancreatic cancer.
Differentiating and confirming signs of pancreatic cancer from other conditions
It can be challenging, as many symptoms are nonspecific and may resemble those of less severe illnesses. However, a combination of medical history, physical examination, and diagnostic tests can help cancer specialists determine the cause of the symptoms.
Here are some steps to differentiate and confirm signs of pancreatic cancer from other conditions:
- Medical history and physical examination: A thorough medical history and physical examination can provide valuable information about a patient’s symptoms and potential risk factors for pancreatic cancer. A Cancer specialist will inquire about the duration, severity, and nature of the symptoms, as well as any personal or family history of cancer or other illnesses.
- Blood tests: Blood tests can help detect abnormalities in liver function, blood sugar levels, and the presence of certain tumor markers associated with pancreatic cancer, such as CA 19-9. However, these tests alone cannot confirm a diagnosis of pancreatic cancer, as elevated levels may also be present in other conditions.
- Imaging tests: Imaging tests such as ultrasound, computed tomography (CT) scan, magnetic resonance imaging (MRI), and endoscopic ultrasound (EUS) can help visualize the pancreas and surrounding structures. These tests can identify tumors, inflammation, or obstructions in the pancreas and help differentiate between pancreatic cancer and other conditions, such as pancreatitis or gallstones.
- Biopsy: A biopsy is the definitive test for diagnosing pancreatic cancer. During a biopsy, a small sample of tissue is collected from the pancreas, usually through an endoscopic ultrasound-guided fine needle aspiration (EUS-FNA). The sample is then examined under a microscope by a pathologist to determine if cancer cells are present.
- Additional tests: In some cases, additional tests may be necessary to differentiate pancreatic cancer from other conditions. These tests may include endoscopic retrograde cholangiopancreatography (ERCP) to examine the bile ducts and pancreatic ducts, or laparoscopy to visualize the pancreas directly.
It is important to consult with a pancreatic cancer specialist if you experience any persistent symptoms or have concerns about your health.
Early detection and intervention can significantly improve the prognosis and treatment outcomes for pancreatic cancer patients.
Must Watch This Video
Advice to patients after diagnosis
After a pancreatic cancer diagnosis, it is important to seek the advice of a qualified GI cancer specialist. A GI cancer specialist can provide personalized guidance and treatments tailored to the individual’s needs.
For early-stage pancreatic cancer surgery is the only treatment that can cure cancer. so timely surgery by a specialist is foremost important.
In addition, patients should take steps to manage their symptoms and help preserve their quality of life.
Here are some tips for patients living with pancreatic cancer:
Follow a healthy diet: Eating a balanced and nutritious diet can improve overall health and help manage symptoms. A nutritionist or registered dietitian can provide guidance on the best foods to eat for pancreatic cancer patients.
Get regular exercise: Regular physical activity is beneficial for all cancer patients, as it helps promote general well-being and reduce fatigue. It is important to consult with a pancreatic cancer doctor and physical therapist before starting an exercise program.
Seek emotional support: Cancer can be a difficult journey, both physically and emotionally. It is important to have open conversations with family members, friends, or medical professionals such as therapists or counselors about any concerns that arise throughout the treatment process. Additionally, patients may benefit from joining a cancer support group or speaking with a mental health professional.
Complementary treatments: Complementary therapies such as acupuncture, massage, and yoga may help reduce stress and relieve pain associated with cancer. However, it is important to discuss any complementary treatments with a doctor before starting them to ensure they do not interfere with medical treatment.
By following these tips, pancreatic cancer patients can improve their quality of life and manage their symptoms.
Diet to Reduce Colorectal Cancer risk
HOME Videos Diet to Reduce Colorectal Cancer Risk AuthorSurgical Oncologist MBBS, MS, MChKnow the...
Thyroid Cancer: Types, Diagnosis & Treatment
HOME Videos Thyroid Cancer: Types, Diagnosis & Treatment AuthorSurgical Oncologist MBBS, MS,...
Does Robotic Surgery Improve Patient survival?
HOME Videos Does Robotic Surgery Improve Patient Survival AuthorSurgical Oncologist MBBS, MS,...
Prostate Cancer: Warning Signs and Early Detection
Prostate cancer warning signs, risk factors, and early detection methods. Common symptoms and when to seek medical attention
Prostate Cancer Treatment: Types, Options, and Side Effects
Prostate cancer treatment: Understand types, options, side effects, and decision-making. Prostate cancer types are adenocarcinoma and neuroendocrine carcinoma.
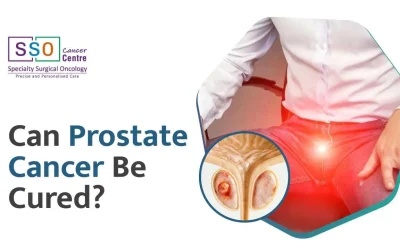
Can Prostate Cancer Be Cured? Treatment and Prognosis
Comprehensive guide on prostate cancer: understanding, treatment options, prognosis, prevention, and ongoing research for informed decisions.


 Blogs
Blogs