Synovial Sarcoma at an unusual and complex site
By Dr. Chetan Anchan
Brief History: Ms. A, 27 yrs. old unmarried lady from northern India noticed a small painless swelling in the pubic region. Over the next few weeks, the swelling grew noticeably.
Within a few more weeks it had increased to the size of an orange and started causing some pain. That’s when she sought medical attention. She was told to see a cancer specialist. All of this took another few weeks. By this time the swelling had become huge and was encroaching on to the vulva.
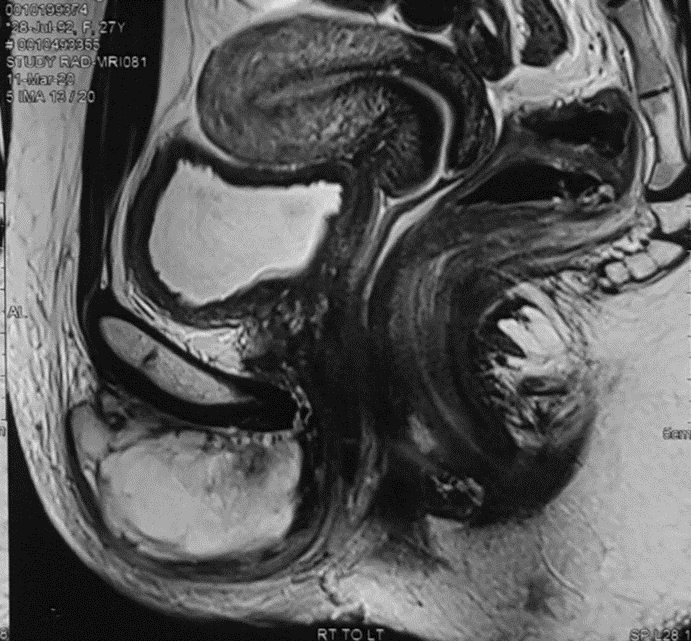
She was imaged and a biopsy was done which confirmed the diagnosis of a high grade sarcoma – synovial sarcoma to be precise. The MRI revealed a large soft tissue mass on the anterior aspect of the pubis curving over the lower edge of the pubic symphysis and entering into the lower pelvis.
The mass was sitting on the urethra and the anterior wall of the vagina, reaching the urinary bladder.
She was told that she will need surgery. But the surgery for tumor resection will involve removal of the urethra, vagina, uterus and the urinary bladder. This was devastating news for her due to which she and her family decided to come to Mumbai for treatment, with the hope of a more acceptable outcome.
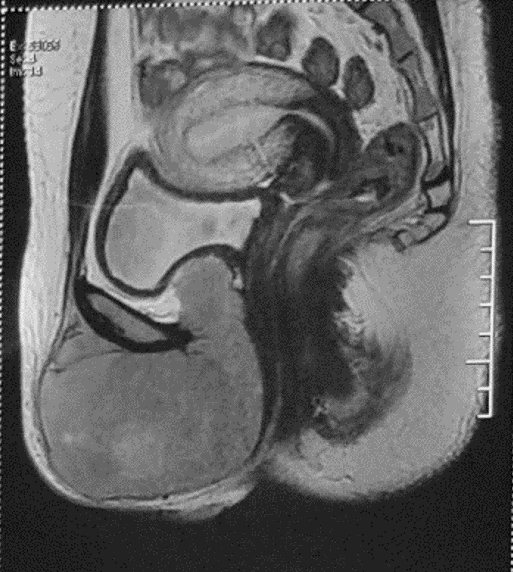
Fig 01. Initial MRI showing a large soft tissue mass anterior to pubis and spreading under the pubic arch and reaching the bladder, urethra and anterior vaginal wall.
Patient Concerns:
When she was first seen by us, the soft tissue mass had grown further and she was finding it difficult to walk; in fact, in a matter of days, she could not walk anymore and had to use a wheelchair. On studying the imaging and on examination, it seemed unlikely that the urethra could be saved. Even the vagina was clearly at risk. If the urethra could not be saved, she would need a permanent stoma with an ileal conduit – a complex procedure where a new urinary bladder is created from a loop of the small intestine and which drains through a hole on the side of the abdomen into a collecting bag.
Treatment Offered:
She was then counselled regarding the disease and the risks involved. Surgery for cancer is a life saving procedure and loss of organs and vital tissue is often a compromise worth making in order to safeguard the life of the patient.
However, this was a young unmarried lady who was on the verge of a mutilating and life changing procedure where she would end up with a permanent stoma for the urinary function. Besides, there was a clear risk of serious and permanent damage to the vagina and related vulval structures.
This is when she was given an alternative option which could give us a shot at saving these structures while safely removing the tumor. We discussed this with her and her family and she agreed to take this chance.
So, unlike what would have been generally planned otherwise, we decided to treat the tumor with radiotherapy before the surgery. This was with the hope that with a good response the tumor could shrink in size and give us a chance at saving the vital structures at risk.
Results of Radiation:
At the time of starting radiotherapy, the tumor was almost 11 to 12 cms. in diameter. She was given 50.4 Grays of radiation over a period of six weeks in 28 fractions; which got over at the end of January this year.
She was asked to follow-up with us after 6 weeks with a fresh MRI for reassessment and surgical planning. In mid March she followed-up with fresh MRI and PET-CT imaging.
The mass had responded very well to the radiation treatment. Her pain had gone down and she was walking again. Now it was time to remove the residual sarcoma with surgery.
Fig 02)Before radiation: 12cm synovial sarcoma in close proximity to bladder, urethra and anterior vaginal wall.
Due to the complex location of the disease and the complexity involved in the surgery, we put up a team of specialist surgeons to operate on her. And just when things were falling in place, the Corona Virus disaster struck.
The whole country was in lockdown and medical services was severly hit. Operating a patient now looked difficult. However, with Ms. A, we had a really narrow window to operate. If we wait too long, her tumor would grow back again and we would lose all the advantage we had now.
It was now or never for us. She was from out of station and had come the city just for her surgery. Now, it looked almost impossible. It was then that we decided not to let this opportunity go. We put up a team of willing surgeons and a brave anaesthetist and operated on her, after explaining her again all the risks involved, although the prospects of getting a good outcome was certainly better now.
Results of the surgery:
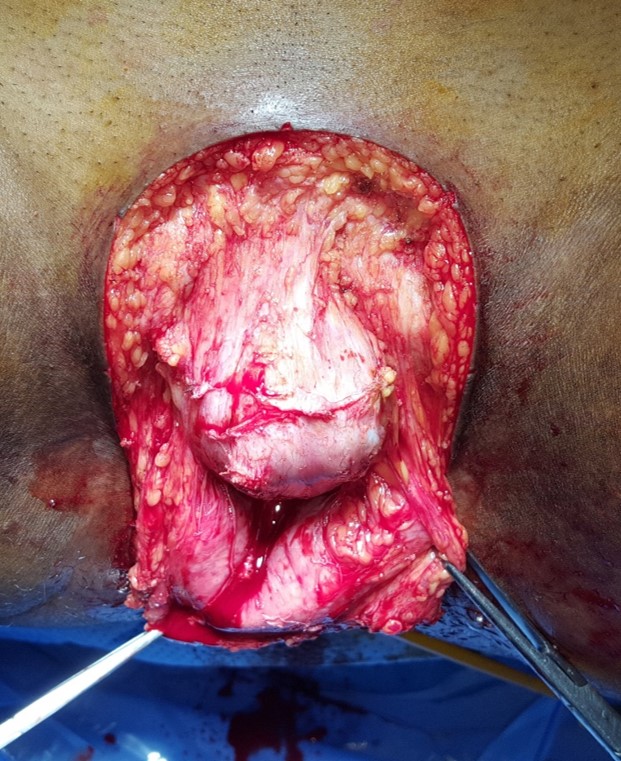
Her surgery went very well. We could save her urethra, vagina, vulval structures and got the tumor out with safe margins all around – as was confirmed in the final histopathology report. Our plastic surgeon inserted a gracilis muscle flap into the defect created in the subcutaneous space to support the pubic skin.
The moment of truth came when the urinary catheter was removed around a week after the surgery. She was having full control over the bladder function. We could not have hoped for a better outcome. She recovered well from the surgery and went home a few days ago.


 Case Studies
Case Studies