Author
Dr. Jay R Anam
Why are Breast Cancer Screening Guidelines So Confusing?

Breast cancer screening is a crucial aspect of women’s health, allowing for early detection and successful treatment. However, guidelines for breast cancer screening can be confusing, leaving many patients and their families uncertain about the best course of action.
In this article, we explore the reasons behind the variation in guidelines, address common concerns and misconceptions, and provide strategies for understanding and navigating these recommendations. We also interview a breast cancer doctor to offer insights into personalized decision-making.
The Reasons Behind Variation in Guidelines
There are several factors contributing to the confusion surrounding breast cancer screening guidelines:
- Different organizations have different recommendations: Organizations such as the American Cancer Society (ACS), the U.S. Preventive Services Task Force (USPSTF), and the National Comprehensive Cancer Network (NCCN) each have their own guidelines for breast cancer screening. These differing recommendations can lead to confusion for patients and healthcare providers alike.
- Evolving research: As new studies emerge, guidelines may change to reflect the latest evidence. This can make it challenging for patients to stay up-to-date on the most recent recommendations.
3.Individual risk factors: Each woman has unique risk factors that can influence the appropriate screening schedule for her. Family history, genetic predispositions, and personal health history can all play a role in determining the best approach to screening.
Breast cancer screening complexities
Breast cancer screening methods, such as mammography, ultrasound, and magnetic resonance imaging (MRI), each have their benefits and limitations.
- Mammography: The most common screening method, mammography uses X-rays to detect abnormalities in breast tissue. While effective for many women, mammography may not be as accurate for those with dense breast tissue, which is common in younger women and those taking hormone replacement therapy.
- Ultrasound: This method uses sound waves to create images of the breast tissue. Ultrasound can be helpful for women with dense breasts or those who cannot undergo mammography, but it may not detect all cancers, especially very early or in situ disease.
- MRI: Using magnetic fields and radio waves, MRI can provide detailed images of the breast tissue. While highly sensitive, MRIs can be expensive and time-consuming and may lead to unnecessary biopsies due to false positives
Addressing Common Concerns and Misconceptions
Several misconceptions and concerns may contribute to the confusion surrounding breast cancer screening guidelines:
- Overdiagnosis: Some worry that increased screening can lead to overdiagnosis, or the detection of cancers that may never become life-threatening. However, early detection can save lives, making it an essential part of breast cancer prevention.
- Radiation exposure: Mammograms do expose patients to a small amount of radiation, but the benefits of early detection generally outweigh the risks.
- Age-related confusion: Different guidelines recommend varying ages at which to begin screening, causing uncertainty among patients. Discussing your risk factors with a healthcare provider can help determine the most appropriate age to start screening.
Must Read This Blog- Myths About Breast Cancer Biopsy Procedure
Strategies for Navigating Guidelines and Practical Tips
To make sense of the various breast cancer screening guidelines, consider the following tips:
- Educate yourself about the different guidelines and the reasoning behind them.
- Discuss your individual risk factors and screening preferences with your healthcare provider.
- Stay informed about the latest research and updates to screening recommendations.
- Consider seeking a second opinion if you are unsure about your provider’s recommendations.
If you are looking for breast cancer treatment then you are in the right place Dr. Jay R. Anam is one of the best breast cancer surgeons in Mumbai
Our Recommendations
Each woman’s situation is unique, and the best approach to screening will depend on her risk factors, personal preferences, and medical history.
It’s essential to have open communication with your breast cancer doctor to discuss these factors and develop a personalized screening plan that works best for you.
By staying educated, discussing your risks with a healthcare provider, and considering expert insights, you can navigate breast cancer screening with confidence.
Diet to Reduce Colorectal Cancer risk
HOME Videos Diet to Reduce Colorectal Cancer Risk AuthorSurgical Oncologist MBBS, MS, MChKnow the...
Thyroid Cancer: Types, Diagnosis & Treatment
HOME Videos Thyroid Cancer: Types, Diagnosis & Treatment AuthorSurgical Oncologist MBBS, MS,...
Does Robotic Surgery Improve Patient survival?
HOME Videos Does Robotic Surgery Improve Patient Survival AuthorSurgical Oncologist MBBS, MS,...
Prostate Cancer: Warning Signs and Early Detection
Prostate cancer warning signs, risk factors, and early detection methods. Common symptoms and when to seek medical attention
Prostate Cancer Treatment: Types, Options, and Side Effects
Prostate cancer treatment: Understand types, options, side effects, and decision-making. Prostate cancer types are adenocarcinoma and neuroendocrine carcinoma.
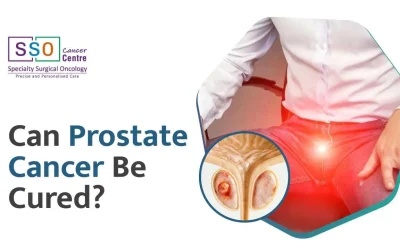
Can Prostate Cancer Be Cured? Treatment and Prognosis
Comprehensive guide on prostate cancer: understanding, treatment options, prognosis, prevention, and ongoing research for informed decisions.


 Blogs
Blogs